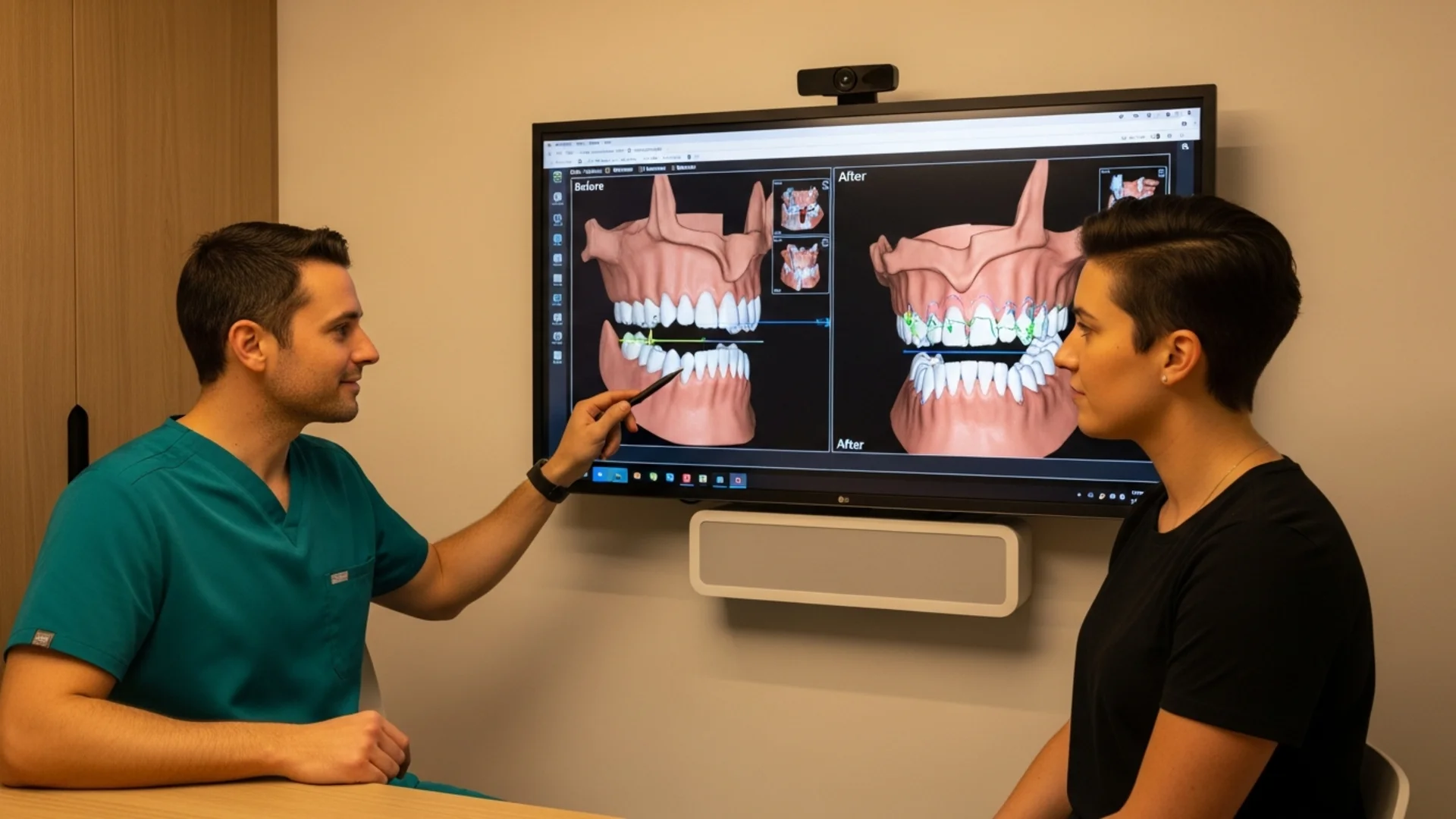
Before — A Bite That Never Worked Right
[PLACEHOLDER] Describe the lived experience of a severe bite discrepancy: chewing fatigue, jaw pain or clicking, sleep disrupted by airway issues, headaches, self-consciousness about a recessed chin or open bite. End on the orthodontist saying braces alone won't fix it.